Why Woman-Centered Midwifery Works
By Joan Tupponce
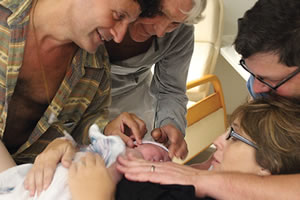 Ivy MacCurtin’s birthing process at The Women’s Hospital this past September was very different than her previous births. The Caroline County mom has three children of her own, ranging in age from six to eleven, and has served as a surrogate three times.
Ivy MacCurtin’s birthing process at The Women’s Hospital this past September was very different than her previous births. The Caroline County mom has three children of her own, ranging in age from six to eleven, and has served as a surrogate three times.
She had her latest surrogate birth in one of the new labor and delivery rooms at The Women’s Hospital at Henrico Doctors’ Hospital with her certified nurse midwife, Amber Price, by her side. Price is also vice president of The Women’s Hospital and an advocate for woman-centered care.
“The difference at The Women’s Hospital is the staff is much more concerned about the birth being more comfortable and homelike. They want to facilitate the type of birth you want,” MacCurtin says.

This time, the baby girl Price delivered was only separated from the birth mother and the baby’s intended fathers (a gay couple from Sedona, Arizona, who were present for delivery) for under an hour while the birth mother was getting checked. “We were given a say in what was done,” MacCurtin says. “I could tell them to bring the baby back to the room so we were able to do everything bedside. After that, everything was done with either me holding her or her dads holding her. Amber [Price] has made positive impacts in keeping the moms and the babies together in the hospital.”

Both the labor-and-delivery and mother-baby units offer the latest technology, which includes the Novii Wireless Patch System, a peel-and-stick patch placed on the mother’s abdomen that wirelessly transmits monitored information such as fetal and maternal heart rates. It replaces the more cumbersome belts that are typically used for monitoring mom and baby.
The Women’s Hospital will also include several departments and specialty units, as well as pediatrics and six gynecologic operating rooms with a da Vinci Robotic Surgical System.
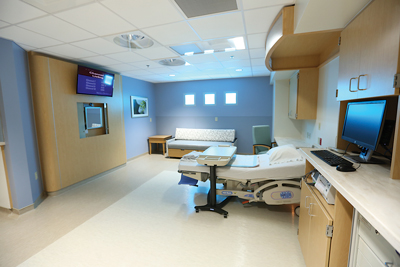
During her stay, MacCurtin had a spacious room that was peaceful and private, but she secretly wished she had scored one of the new king suites to accommodate the welcome-to-the-world party for the baby she had just birthed. “My husband and I and the baby’s parents were all in one big room,” she says.
The king suite rooms, with their king-size beds, promote a family-centered recovery. “The husband gets to stay and sleep in the same bed with his wife like they do at home,” says Price. “We also have deep Mandarin soaking tubs that have hydrotherapy for labor pain.”
While planning the concept for the hospital, Price and her team had the opportunity to think about what women are looking for when they give birth, as well as when they need medical services. “This is woman-centered care with options and choices across the spectrum of women’s health through their lifetime. It includes everything from the totally normal to the complicated,” she says. “Here the woman is central to the decision-making process surrounding her care.”
Hospital staff members focus on living by the platinum rule of treating others the way they want to be treated “and thereby treat every woman as an individual with unique expectations of her care,” Price says. “We have undergone a cultural change as we moved from a traditional care model to a family-centered care model where mothers and infants and their family members stay together throughout their hospital stay, regardless of how their births occurred – cesarean or vaginal.”

Some women are terrified of labor, for example, and want a cesarean birth for fear of a long, painful labor. “They want someone to keep them safe,” Price says. “We accommodate those women, as well as women who don’t want any interventions at all. We accommodate a full range of requests.”
Midwifery is a specialty
Essential to the hospital’s services are midwifery and low-intervention births. “Eighteen to 20 percent of women in our community are interested in low-intervention birth,” says Price, who delivered the facility’s first hospitalist midwife baby in December 2015. “Since then, we have seen a steady increase. We have delivered more than 180 babies through midwifery.”
There are two different types of midwives – certified professional midwives who are trained only for home births, and certified nurse midwives. The latter are graduate-trained nurses who work in a hospital setting and have a collaborative relationship with physicians. “They can manage all of a woman’s care, and they have a collaborative relationship with a specialist if something falls outside of normal,” Price says of certified nurse midwives.

The hospital focuses on a team approach to treating patients. “We’ve worked hard to make this part of a team, and it has been this really friendly, collaborative environment. You don’t have to leave your doctor to go to another practice. This [midwife] practice is like Switzerland,” Price says. “It’s neutral and available to any physician practice that chooses to participate. In other places, midwifery is a different practice. It pulls patients away from their physician practices.”
For MacCurtin, giving birth through a midwife is empowering. “Having a midwife like Amber who I trust one hundred percent is absolutely wonderful. You know they are not going to steer you the wrong way,” she says. “Their interest is for you and your baby, and not what is most convenient for the hospital.”

Certified nurse midwife Lois Hancock, who practices midwifery at the hospital, remembers how vulnerable she felt as a young woman giving birth decades ago, and how education changed her outlook. “Through reading, and then taking Lamaze classes, I became aware of choices I could make for myself while in labor,” she says. “This improved my birth experiences dramatically. After that, I wanted to empower other pregnant women by making knowledge and options available to them.”
Over the course of her career, Hancock has birthed more than 1,600 babies. The heart and soul of the midwife “is to be with a woman in her travail of labor and birth – to hear her, to respect her preferences, to affirm her choices, and mainly, to support her through the process of giving birth,” Hancock says. “We, as midwives, are not to dictate to the woman what she should be doing in the act of giving birth. This is the pregnant woman’s birth experience, and I want her to feel heard and respected.”
Hancock came to The Women’s Hospital this summer after working in Tidewater because she believes the hospital is more of a true model of midwifery. “The model of care here allows me to be there for my patient throughout the entire event of birth,” she says.
Women who want to give birth at the hospital are encouraged to tour the facility as well as take childbirth classes so they can get a clear idea of their choices before they go into labor.

Being part of the birth journey – seeing women become mothers and people becoming families – is an honor for her. “As a woman, I think everybody is entitled to make informed decisions and be supported,” she says of the birth process. “That’s why I like being here. I feel like the changes here at the hospital are really about giving women those options.”
Henrico resident Stephanie Lau gave birth to her first child, a little boy named Aidan, on September 13 at the hospital. Early in her pregnancy, she had decided she wanted a low-intervention birth with a midwife, but she also kept seeing her doctor in the OB/GYN practice she used. “I figured if I did have to have a medical intervention, it would be with a provider I knew,” she says.
Much to her surprise and good fortune, her delivery was short, only about six hours. “I was nine centimeters, when we got to the hospital,” she says. “I was there for an hour, and was able to deliver immediately.”
Batten was the midwife who attended the birth. “She stayed after the birth to make sure I was comfortable and breastfeeding okay,” Lau says. “She visited me during recovery. I was able to stay in a king suite and keep our child with us. He didn’t go to the nursery unless we requested it. Having that environment was great. It didn’t feel like a hospital. It felt more like a hotel stay with nurses checking in.”